Content for TR 22.826 Word version: 17.2.0
5.3.4 Mobile Specialist Practice
5.3.4.1 Description
5.3.4.2 Pre-conditions
5.3.4.3 Service Flows
5.3.4.4 Existing features partly or fully covering the use case functionality
5.3.4.5 Potential New Requirements needed to support the use case
...
...
5.3.4 Mobile Specialist Practice p. 37
5.3.4.1 Description p. 37
Healthcare systems in developed countries currently face a strong trend towards concentration of care in large hospitals located in urban centers. This is on one hand due to efficiency/cost reasons and on the other hand due to a simple lack of skilled experts. Some studies even state that small rural clinics with very limited possibilities for examination or treatment might be dangerous for patients with serious diseases due to the lack of expertise. This concentration leads to huge travel efforts even in rather standard cases like aftercare examinations, screenings or medical check-ups. In addition to that, these large hospital centers today also have to provide care for emergency cases, which means that standard cases get lower priorities and thus, long waiting times are quite usual.
Many of the aftercare examinations, screenings or medical check-ups do not necessarily require an expert who is locally present during the exam if a broadband, low latency and high quality of service data link would be available. In this case video examinations based on high end camera and audio systems (even supported by haptic feedback if necessary), remote diagnosis of imaging data from ultrasound, X-ray, computed tomography or even magnetic resonance imaging could be conducted by a "remote expert". In order to provide such remote expert examinations, the following features need to be in place:
1)
A mobile specialist practice which is located in a truck. It may contain
- an examination room with high end video/audio equipment which can establish a broadband connection to an expert located in a remote location
- optionally a set of medical imaging equipment like ultrasound, X-ray, CT or even MRI all capable of connecting to a dedicated 5G network and transmitting diagnostic data in real time to the remote expert
- optionally mobile lab diagnostic equipment
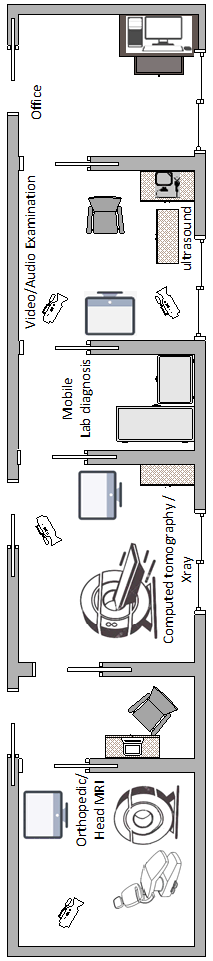
2)
A country-wide network of dedicated non-public network (NPN) 5G access points owned by communities or other service providers, or a corresponding private slice. Once the mobile specialist practice arrives at the access point and checks in, the necessary network resources according to the examinations schedule are allocated.
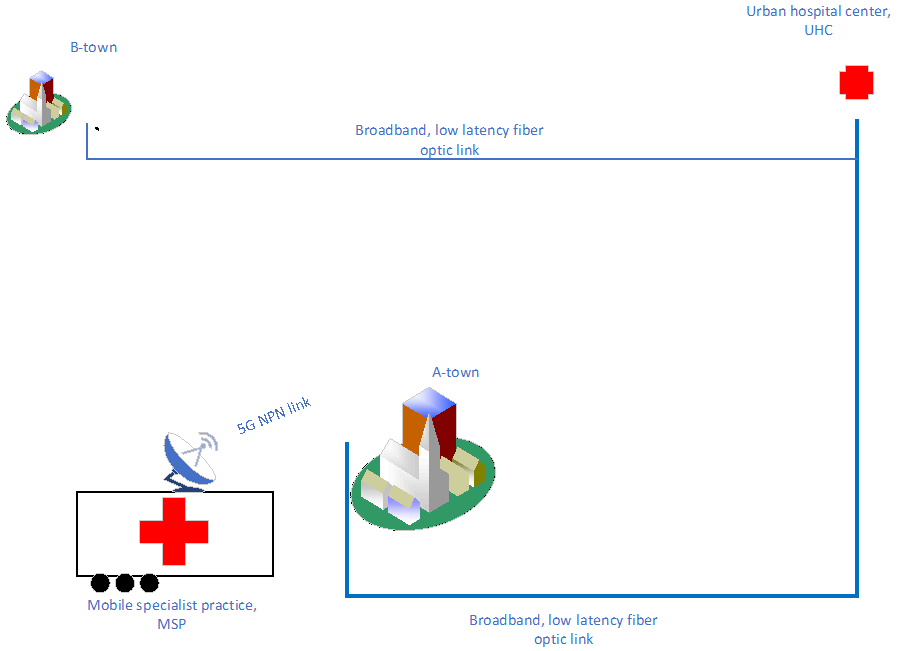
3)

In order to make such a mobile specialist practice an efficient and accepted part of tomorrow's healthcare system it is key that it is patient centered. That means that currently well-known nuisances like long waiting times for appointments, long waiting times due to inefficient planning or emergencies or non-ideal communication need to be avoided. Thus, one of the key features of such a mobile specialist practice is the scheduler which works in the background. A further very important factor is trust: it needs to be guaranteed, that the patient contacts as many virtual experts as necessary but as few as possible - the well-known annoying call-center situation with a new "expert" in every new call is a no go. It also needs to be ensured that the patient keeps informed about each step of the examination, that he gets information about the experts he is connected to and that the procedure ends with a satisfying outcome - either the patient is cured or a longterm treatment plan has been defined.
An efficient scheduler to align all required resources:
- Patient appointment
- Allocation of necessary equipment (might be added on demand for non-common cases)
- Local staff, e.g. MTAs or paramedics
- Remote specialist
- Network resources (reserve links with appropriate bandwidth, latency and QoS for each planned examination)

5.3.4.2 Pre-conditions p. 39
One day about one year ago, Mark recognized a strange change of a small region of his skin on his right arm. As it didn't dissolve within some weeks and he even observed some progression, he made an appointment at Dr. Good, a dermatologist in the large city next to his home town. Although he was rather flexible, it took about 6 weeks to get one and as it was in the middle of the day, he had to take one day off work to drive there. All in all, this first appointment took almost all day long including driving, waiting and the examination, which was a small biopsy surgery. About one week later he called Dr. Good's practice for the result and was told that it was in fact white skin cancer which afforded a surgical removal. Two weeks later the surgery was carried out successfully and the dermatologist suggested a quarterly screening to monitor the healing process and check for further lesions. When Mark pointed out that each screening necessarily means a whole day off work for him, his dermatologist suggested to make use of the new mobile specialist practice (MSP), for which Dr. Better - a good friend of him and an experienced dermatologist, too - works as a remote expert regularly.
A few weeks later, Mark called the phone number that was given to him by his dermatologist. He also had agreed that his patient data including the report on his recent surgery have been uploaded to his private medical data account and made accessible for Dr. Better. After a very short phone interview he got a 10 o'clock appointment for a skin cancer screening carried out at a mobile specialist practice (MSP) only about 3km away from his work office. The day of his examination he left his office and went to the MSP by bike. Arriving there, a paramedic already awaited him, the video/audio examination room was prepared and Dr. Better, the remote expert, was online. Due to the information provided in Mark's medical data account, Dr. Better was well prepared and knew about Mark's previous surgery. After a short introduction and some brief information about the following procedure, the visual whole-body screening started. Mark followed the instructions given by Dr. Better including the placement of a haptic manipulator on the location of his recent surgery. After remotely palpating this area the examination was finished without any new findings. Dr. Better explained the examination results to Mark and gave him some recommendations on skin care especially for the location of his recent surgery. Based on the video stream a documentation of the screening in order to compare to future changes was created automatically and added to Mark's medical data record. Mark left and was back at his office shortly after 10:30, being sure to use the MSP again for his next regular screening.
5.3.4.3 Service Flows p. 39
The mobile specialist practice arrives at the predefined location with a community owned non-public-network access point and connects to it. Based on a service level agreement the data links needed according to the day's schedule are allocated for the MSP. At 10 am, a visual whole-body skin cancer screening is scheduled and the required resources are allocated and connected to the NPN wireless network.
- In the video/audio examination room, a stereoscopic video camera with optical zooming produces a 4K video stream while an audio system enables EVS full band voice communication with the remote specialist. The video (stereoscopic 4K 60 fps 12 bits per pixel color coded (e.g. YUV 4:1:1) real time, loss less compressed video) and the audio stream (up to 128 kbit/s) are relayed by the MSP to the remote specialist located in the next urban hospital center. A second video stream with lossy compression from remote expert to the MSP is available to ease communication with the patient via a 4K monitor in the MSP's examination room. A haptic feedback tool for remote palpating is connected via a low latency link with 2 Mbit/s from network to UE and 16 Mbit/s from UE to network.
- Resources assigned for the communication services allocated to the skin cancer screening are released after the examination. At 10:30 am a knee MRI scan and an abdominal ultrasound are planned.
-
New resources for the next examination(s) are allocated:
- for the MRI scan, a standard video conferencing link, a 50 Mbit/s low latency link to share the scanner's console and a 240 Mbit/s broadband link to upload a 300 Mbyte DICOM file in less than 10 seconds are allocated. The remote radiologist gives a brief introduction to the patient and some scan instructions to the MTA. After the scan has finished, the raw data are processed in the MSP and a complete DICOM data set is uploaded to the remote specialist for immediate diagnosis.
- for the ultrasound examination, which is done in parallel, a second standard video conferencing link and a 160 Mbit/s link to transmit an uncompressed 512x512 pixels 32 bits 20 fps video stream from an ultra-sound probe are allocated. The remote specialist gives a brief introduction to the patient and continuous scanning instructions to the paramedic in the MSP. The diagnosis is given during or immediately after the examination via the video conferencing link.
- Resources assigned for the communication services allocated to MRI scan and the ultrasound examination are released after the examination. Other examinations such as CT-scan, blood analysis follow a similar, respective service flow. Each medical device contains a 5G UE. Each medical device may connect to the 5G network directly, or the medical devices connect to the local 5G non-public network of the mobile specialist practice. The mobile specialist practice has a connection to the 5G network (private slice) for the connection to remote specialists etc.
5.3.4.4 Existing features partly or fully covering the use case functionality p. 40
| Reference number | Requirement text | Application / Transport | Comment |
|---|---|---|---|
| 8.9 | The 5G system shall support data integrity protection and confidentiality methods that serve URLLC and energy constrained devices. | T | See TS 22.261 |
| 6.1.2 | All requirements related to slice management, access, capacity, quality of service. In particular, on prioritization of certain slices against others: The 5G system shall enable the network operator to define a priority order between different network slices in case multiple network slices compete for resources on the same network. | T | See TS 22.261 |
| 6.10.2, 6.1.2.3 | All requirements related to private slice management, access, limitation to a specific geographical area, isolation and fault tolerance. | T | See TS 22.261 |
| 8.2, 8.3 | All requirements related to security management in private slices | T | See TS 22.261 |
| 6.2.3 | The 5G system shall enable packet loss to be minimized during inter- and/or intra-access technology changes for some or all connections associated with a UE. | T | See TS 22.261 |
| 6.2.3 | The 5G system shall minimize interruption time during inter- and/or intra- access technology mobility for some or all connections associated with a UE. | T | See TS 22.261 |
| Video/Audio streams of video conferencing, video supervision. | T |
5.3.4.5 Potential New Requirements needed to support the use case p. 41
| Use case | Characteristic parameter | Influence quantity | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Mobile specialist practice | Communication service availability: target value in % | Communication service reliability: Mean Time Between Failure | End-to-end latency: maximum | Bit rate | Direction | Message Size [byte] | Survival time | UE speed | # of active UEs (Note 1) | Service Area [km2] (Note 2) |
| Stereoscopic 4K 60 fps 12 bits per pixel color coded (e.g. YUV 4:1:1) real time video (loss less compressed) | 99.99 | > 1 month | < 250 ms | 2 Gbit/s | UE to Network | ~1500 -9000 | ~16 ms | stationary | <20 per 100 km2 | ~ 0.1 Regional |
| Compressed 4K video stream | 99.99 | > 1 month | <100 ms | 25 Mbit/s | Network to UE | ~1500 | ~100 ms | stationary | <20 per 100 km2 | ~ 0.1 Regional |
| Haptic feedback data stream | 99.999 | >> 1 month (< 1 year) | <20 ms | ~2 Mbit/s / 16 Mbit/s | UE to Network; Network to UE | ~80 | ~1 ms | stationary | <20 per 100 km2 | ~ 0.1 Regional |
| High quality audio stream | 99.99 | > 1 month | <100 ms | 128 kbit/s | UE to Network; Network to UE | ~300 | ~16 ms | stationary | <20 per 100 km2 | ~ 0.1 Regional |
| CT/MRI scan data, max 300Mbyte of DICOM data | 99.99 | > 1 month | seconds | >240Mbit/s | UE to Network | ~1500 - 9000 | stationary | <20 per 100 km2 | ~ 0.1 Regional | |
| Remote console for CT/MRI (XVGA compressed) | 99.99 | > 1 month | <100ms | 50Mbit/s | Network to UE; UE to Network | stationary | <20 per 100 km2 | ~ 0.1 Regional | ||
| Uncompressed 512x512 pixels 32 bits 20 fps video stream from ultra-sound probe | 99.99 | > 1 month | <50 ms | 160 Mbit/s | UE to Network | ~1500 | ~50 ms | stationary | <20 per 100 km2 | ~ 0.1 Regional |
|
NOTE 1:
UEs per type of communication service. The use case has approx. 12 UEs supporting different applications / communication services.
NOTE 2:
The mobile specialist practice has dimensions of ca. 15 m x 3 m x 3 m. However, the UEs need to connect to the base station of the 5G network in the vicinity. The complete service area is regional (from mobile specialist practice to remote specialist in hospital)
|
||||||||||