Content for TR 22.826 Word version: 17.2.0
5.3 Static - Remote
5.3.1 Description of Modality
5.3.2 Emergency care - Ultrasound examination and remote interventional support
...
...
5.3 Static - Remote p. 28
5.3.1 Description of Modality p. 28
This modality is about Telemedicine, whose definition as adopted by the World Health Organization is as follow:
"The delivery of health care services, where distance is a critical factor, by all health care professionals using information and communication technologies for the exchange of valid information for diagnosis, treatment and prevention of disease and injuries, research and evaluation, and for the continuing education of health care providers, all in the interests of advancing the health of individuals and their communities".
The main difference between Telemedicine and Telehealth is that products and services offered as part of Telemedicine are regulated by Health laws. This is important to understand that as by their intrinsic nature, those services may cross national boundaries and regulatory systems.
According to [18], global healthcare expenditure continues to increase. In fact overall healthcare spending is expected to grow from 7 trillion USD in 2015 to almost 9 trillion USD in 2020, with estimated CAGR of 4.3 %. In addition, long term projections forecast a further increase to more than 18 trillion by 2040. However, growing healthcare needs due to global population aging, prevalence of dementia and chronic diseases, are not compensated by the increased expenditure even in developed countries due to operational difficulties, regulatory burdens and financial inefficiencies. As noted in [19], this leads to experiencing decreased healthcare service accessibility due to global shortage of general and specialist staff that increases patients waiting times and affects their ability to access to diagnosis and treatment.
On the one hand, increasing the number of care workers can only be a partial solution to this problem as it does not allow to contain costs. And on the other hand, the technology and especially Telemedicine and mobile health, with its potential to improve physician access, add flexibility and capacity to specific healthcare services, can greatly help at reasonable costs. This translates into high market value for Telemedicine, estimated at $18 billion in 2015 and expected to increase over $40 billion in 2021 according to [20].
This chapter contains use cases and requirements showing how, in practice, the 5G system can help decoupling location from quality of care, and save countless hours for doctors and surgeons, who will be able to "beam" themselves to operating rooms, incident sites and medical houses, rather than having to be physically present.
In those use cases, special attention is paid to patient safety and confidentiality. In practise, the data being communicated needs to be fully encrypted and integrity protected, which requires additional computing bandwidth on both ends.
5.3.2 Emergency care - Ultrasound examination and remote interventional support p. 28
5.3.2.1 Description p. 28
Ultrasound is an opportunity for emergency care in the ambulance. It significantly improves the management of prehospital care (first diagnosis, intervention and triage) and reduces the "door to diagnosis and therapy time", which is one of the most important factors in improving medical assistance and survival (as described in [27]):
- Examination must be rapid, not more than 2-3 minutes. For example, pre-hospital focused assessment with sonography in trauma usually takes no more than 3 minutes
- Identification of lung sliding to diagnosis pneumothorax, and the evaluation of abdominal aorta usually lasts less than 1 minute. Heart studies during cardiopulmonary resuscitation should be performed in 10 seconds during the rhythm check.
- The exam should answer specific yes/no questions, i.e., Is there a pneumothorax? Is there free fluid in the pleura, pericardium and peritoneum? Is there an aortic aneurism? Are the lungs wet or dry?
- Trauma, respiratory insufficiency, shock, cardiac arrest and severe abdominal pain, prior medical records should all be used to rule in or rule out an abdominal aortic aneurism
- Pre-hospital triage, airway management, obstetric emergencies
- Category A Red 1 calls, that cover cardiac arrests and patients who are not breathing anymore.
- Category A Red 2 calls, which are serious but less immediately time critical and cover conditions like stroke and fits.
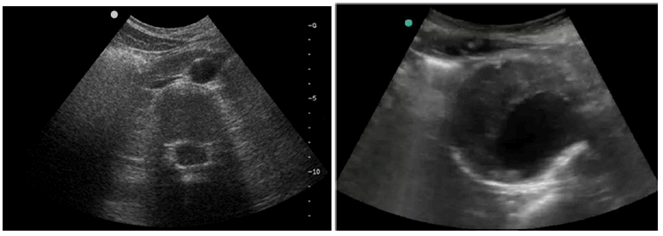
Figure 5.3.2.1-1: Ultra-sound imagery of an abdominal aortic aneurysm (right hand side picture)
(⇒ copy of original 3GPP image)
(⇒ copy of original 3GPP image)
This test is reliable, efficient but however requires some level of expertise not always available on the site of the incident as many first responders have no, or only basic training in echography. This leads to having paramedics in the ambulance performing the echography with the assistance from a remote expert who is able to guide them through the examination procedure. Efficient support involves being able to track paramedics gestures with enough precision, therefore sets limits on the acceptable latency while going thought all equipment along the path from the ambulance to the monitor in front of the expert. In general, we consider here gestures executed at the speed of 30 cm/s and with an expected accuracy of 1cm which gives us a total imaging system latency of up to 35 ms. Along the same principles as depicted in clause 5.2.1.3, but considering there isn't any heavy processing at the application side, one ends up with a below 20 ms one way end-to-end latency from the echographer to the application at the remote expert site.
In a conservative approach for estimation of the communication service availability, consecutive frame loss or delays beyond service defined constraints shall only occur with a very low probability for the duration of the examination.
5.3.2.2 Pre-conditions p. 30
Joe, 78 years old, fell in his basement. The fall detector in his Personal Emergency Response System device (PERS-device) alerted the call centre but as they could not get him to respond they dispatched an ambulance. The ambulance must be equipped with devices for monitoring, examination and guided interventions like e.g. ultrasound probe, physiological signals monitors and, portable 4K smart glasses. Also instant access to medical records is important to understand the patient's condition prior to the incident.
The Emergency Room (ER) and a local MNO have business contract in place by which the ER can ask the MNO (through suitable APIs) to allocate the necessary high priority resources fulfilling SLAs suitable to the transport of medical data (with special care taken on medical data integrity and confidentiality) over a geographical area covering the site of the incident.
Each needed equipment (ultrasound probe, monitoring scopes, 5G enable 4K smart glasses …) is:
- Powered up,
- Subscribed to 5G communication services fulfilling agreed SLAs,
- Attached to the local MNO 5G network,
- Provisioned with parameters allowing establishment of a secure communication link to an authenticated application in the ER and/or hospital in charge of sharing incident data with the authorized personnel
5.3.2.3 Service Flows p. 30
With the ambulance, Fred, the first-aid caregiver arrived on scene and found Joe in the basement. Joe is conscious but complains about intense abdominal pain.
- To check for internal bleeding and lung punctures, Fred pulls out his portable Ultrasound-device (US-device), which directly starts streaming securely ultrasound-data (US-data) to the Emergency Room (ER) through a 5G communication service fulfilling agreed SLAs, where it is analysed by Marc, the sonographer on call. The 2D US-data is a 20fps 512x512 pixels uncompressed image stream encoded using 32bits per pixel.
- To allow Marc to provide optimal instructions on placing the US-probe, Fred also streams live 4K video of Joe's abdomen through the 5G wireless camera mounted on his smart glasses. The video is encoded using 12 bits per pixel color coding (e.g. YUV 4:1:1 [28]), supports up to 60 fps and is compressed with lossy compression algorithm. Based on the video and US-streams, Marc provides instructions to Fred (possibly using a video communication link) how to move the US-probe to assess Joe's abdomen (as an option Marc may even control a robot in the ambulance for the ultrasound capture.). Interactions between Fred and Marc (incl. the 4K video stream and the return communication link) are supported by a second 5G communication service with suitable SLAs. Apart from moving, Marc is able to control the operation of the US-device, e.g. to tune remotely the beam-forming parameters.
- Seeing the ultrasound stream, Marc concludes abdominal aortic aneurysm fissure by noticing fluid accumulation in Joe's abdomen and a heterogeneous rounded ultrasound structure with an anechoic image corresponding to the light of the vessel at its centre. Marc concludes that Joe's condition is critical. Marc tells Fred to ask the driver to get Joe to the nearest hospital at the highest possible speed. Also Marc coaches Fred to use his fist to apply pressure to a specific point based on ultrasound guidance on Joe's abdomen to limit the bleeding.
- Upon arrival at the hospital, the staff is waiting, the OR has been prepared and Joe is rushed there for immediate surgery. Resources assigned to communication services allocated to the Emergency Room are now released by the MNO.
5.3.2.4 Post-conditions p. 31
The surgeon replaces the aorta with a vascular prosthesis that is sewn to the healthy aorta above and below the aneurysm. The surgery procedure is fully successful and Joe is kept under continuous surveillance in the hospital during eight days.
5.3.2.5 Existing features partly or fully covering the use case functionality p. 31
| Reference number | Requirement text | Application / Transport | Comment |
|---|---|---|---|
| 8.9 | The 5G system shall support data integrity protection and confidentiality methods that serve URLLC and energy constrained devices. | T | See TS 22.261 |
| 6.1.2 | All requirements related to slice management, access, capacity, quality of service. In particular, on prioritization of certain slices against others: The 5G system shall enable the network operator to define a priority order between different network slices in case multiple network slices compete for resources on the same network. | T | See TS 22.261 |
| 6.10.2, 6.1.2.3 | All requirements related to private slice management, access, limitation to a specific geographical area, isolation and fault tolerance. | T | See TS 22.261 |
| 8.2, 8.3 | All requirements related to security management in private slices | T | See TS 22.261 |
5.3.2.6 Potential New Requirements needed to support the use case p. 32
| Use case | Characteristic parameter | Influence quantity | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| 5.3.2 - Ultrasound examination & Remote Interventional Support | Communication service availability: target value in % | Communication service reliability: Mean Time Between Failure | End-to-end latency: maximum | Bit rate | Direction | Message Size [byte] | Survival time | UE speed | # of active UEs | Service Area [m2] (note 1) |
| Compressed 4K (3840x2160 pixels) 60 fps 12 bits per pixel color coded (e.g. YUV 4:1:1) real-time video stream | 99.99 | >1 month | <20 ms | 25 Mbits/s | UE to Network | ~1500 | ~100 ms | stationary | <20 per 100 km2 | <50 |
| Uncompressed 512x512 pixels 32 bits 20 fps video stream from ultra-sound probe | 99.999 | >>1 month (<1 year) | <20 ms | 160 Mbits/s | UE to Network | ~1500 | ~50 ms | stationary | <20 per 100 km2 | <50 |
|
NOTE 1:
Straight line distance between an ambulance and the closest emergency room
|
||||||||||